By Jason E. Lowenstein, MD
Jason E. Lowenstein, MD is the Medical Director of Scoliosis and Spinal Deformity for Atlantic Health System and Chief of Scoliosis and Spinal Deformity at Morristown Medical Center. He is also Assistant Professor of Orthopedic Surgery at NYU Langone Health. He received his Bachelor of Arts from the University of Pennsylvania, Medical Degree from the University of Pittsburgh, residency in Orthopedic Surgery from Columbia University Medical Center/New York-Presbyterian Hospital, and fellowship in pediatric and adult spine surgery at Emory University Medical Center.
Adolescent idiopathic scoliosis remains one of the most common diagnoses requiring surgical treatment of the spine in the pediatric population. The gold standard for the past century has been to perform a spinal fusion for treatment of progressive and severe scoliosis. Spinal fusion often includes instrumentation, with the goal being to obtain correction of the patient’s curve in the operating room using screw and rod constructs to straighten the spine, along with a spinal fusion being performed, which attempts to join the bones in the back together. This procedure allows the curve to be corrected and straightened, but comes at the expense of stiffening the spine with the fusion, which results in loss of range of motion.
Introduction to Vertebral Body Tether (VBT)
Vertebral Body Tether has been introduced as an alternative to spinal fusion for surgical treatment of scoliosis. It utilizes the placement of screws into the anterior vertebral bodies, but instead of using a stiff metal rod to correct the scoliosis, it uses a flexible cord (the tether) to obtain correction of the patient’s scoliosis. The screws are placed on the convexity of the curve (the outside of the curve) and the screws are compressed along the cord, allowing for correction of the patient’s scoliosis (Figure 1.) As well, the best results are obtained in the growing spine, and as the outside of the curve is “tethered”, it encourages the inside of the curve to grow faster than the outside, allowing continued correction of the scoliosis after the implants are placed.
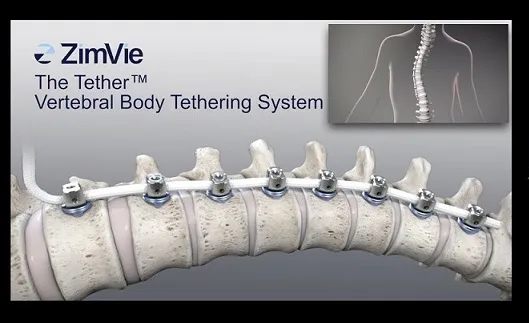
Figure 1
Evolution and FDA Approval of VBT Devices
Vertebral Body Tether, also known as Anterior Scoliosis Correction, was introduced in the last decade, originally using existing spine instrumentation in an “off label” approach. In late 2019, Zimmer-Biomet (ZimVie) obtained FDA approval for their novel device, “The Tether” which was the first FDA approved VBT device to be released in the US. This device was designed specifically for flexible scoliosis correction in the pediatric spine, with indications to include progressive curves between 40 and 65 degrees, and to be used in skeletally immature patients. A second VBT device, Reflect, from Globus Medical, received FDA approval in May of this year.
Comparing VBT and Spinal Fusion: Surgical Techniques
VBT differs from fusion in terms of its surgical approach. While fusions can be done from a lateral approach, the most common current approach is an open posterior exposure, reflecting the paraspinal muscles off the posterior spine to place hardware, obtain curve correction, and perform the spinal fusion by laying bone graft over the decorticated posterior spinal elements. VBT however is done utilizing a minimally invasive approach. In the thoracic spine, video assisted thoracic surgery (VATS) is employed, using an endoscopic approach to visualize the thoracic spine and place instrumentation. In the lumbar spine, additional tubular retractors or “mini-open” exposures are used to access the lateral spine through a retroperitoneal approach. Muscular attachments to the spine are preserved, minimizing post-op pain and improving return to daily activities. In VBT, no fusion is performed, and screws are placed along the convexity of the curve, followed by tensioning of the tether between the screws to allow for correction of the patient’s curve. As a result, patients can mobilize more quickly in the early post-op period and return to normal activities faster as there in no fusion waiting to heal in VBT. VBT is done using a multidisciplinary approach, with the team typically including the orthopedic spine surgeon or neurosurgeon working alongside a thoracic surgeon skilled in the use of VATS approaches.
Initial Adoption and Challenges
Quickly after The Tether was released in late 2019, the Covid-19 pandemic occurred, slowing the initial adoption of this new technique. In 2021, Dr. Federico Steiner (Thoracic Surgery) and I performed the first Vertebral Body Tether in New Jersey at Morristown Medical Center / Goryeb Children’s Hospital utilizing ZimVie’s FDA approved device, The Tether. While there are other groups performing VBT in surrounding states and across the country, we remain the only team in NJ performing VBT with The Tether from ZimVie. (Figure 2a and 2b highlights a 16 yo patient of ours who underwent VBT for treatment of scoliosis.)
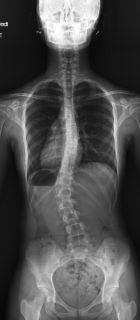
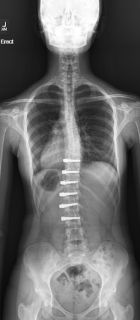
Fig 2a and Fig. 2b
Tether Breakage: Incidence and Management
VBT has a higher complication rate when compared with fusion, with tether breakage being the most common complication (1). The incidence of tether breakage is approximately 20% (2). The tether is radiolucent, so breakage is identified when the angle or distance between two or more screws changes, or the curve worsens between two consecutive x-rays. It is rare for the breakage to result in pain. Not all tether breaks require surgical correction, but if the breakage occurs along with worsening scoliosis, revision surgery can be performed, with either a revision VBT vs. consideration of converting to a spinal fusion.
Motion Preservation in VBT: Lumbar vs Thoracic
Recent studies have shown the relative motion preserved from VBT is significantly greater when performed in the lumbar spine compared to the thoracic spine. Studies have shown that almost all sagittal motion and up to 50% coronal motion is preserved after lumbar VBT, in contrast to thoracic VBT where significantly less motion can be identified post-surgery (3). The thoracic spine has less motion than the cervical or lumbar spine, likely due to the rib attachments to the spine and sternum. Because of the increased risk of tether breakage, and the decreased motion preserved with thoracic VBT, many scoliosis surgeons have forgone performing thoracic VBT and have focused on performing tethers in the lumbar spine. While many patients have both thoracic and lumbar curves that require surgical treatment, hybrid VBT-Fusion procedures have become an option, allowing for correction of the flexible lumbar spine with the motion sparing Vertebral Body Tethering, coupling this with a more predictable posterior spinal fusion for the thoracic curve. We have adopted this approach for our double major curves at MMC and have been very pleased with our outcomes. (Figure 3a and 3b illustrate a 17 yo patient of ours who underwent a hybrid proximal posterior thoracic fusion and distal thoracolumbar VBT.)
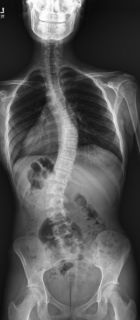
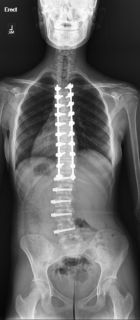
Fig. 3a and 3b
The Future of Vertebral Body Tethering
Vertebral Body Tethering is an exciting and novel minimally invasive approach to scoliosis treatment, allowing for improved patient motion after surgical correction and faster return to activities post-surgery. Hybrid approaches, utilizing posterior fusion in the thoracic spine and VBT in the lumbar spine may be considered when double curves are present, to minimize the risk of tether breakage in the thoracic spine where the spine is already stiff and less motion is present, and to continue to preserve motion in the more inherently flexible lumbar spine.
1.Vertebral body tether for idiopathic scoliosis: a systematic review and meta-analysis. MJ Roser, et al. Spine Deform. 2023 Nov; 11(6): 1297-1307
2.What happens after a vertebral body tether break? Incidence, location, and progression with five-year follow-up. MJ Yang et al. Spine, 2023 Jun 1;48(11):742-747.
3.Measurable lumbar motion remains 1 year after vertebral body tethering. Smitha, EM et al. J Pediatr Orthop. 2022 Sep 1;42(8):e861-867.
